Overview
Peripheral neuropathy is a type of disorder of nerve(s) apart from the spinal cord and brain. Patients with peripheral neuropathy may have numbness, tingling, surprising sensations, weakness, or burning pain in the influenced region. Generally, the indications are balanced and include two hands and feet. Since the symptoms are frequently present in the spaces covered by gloves or stockings, peripheral neuropathy is often portrayed as having a ‘glove and stockings’ delivery of symptoms.
Peripheral neuropathy can include diverse nerve types, including sensory, autonomic, and motor nerves. Peripheral neuropathy can likewise be classified by the size of the nerve fibers included small, or large.
Neuropathy can be present with many varying symptoms, including numbness, the pain of various kinds, loss of balance, or weakness, depending upon the sort of nerve included. Since the autonomic nerves control substantial capacities that we do not deliberately consider, for example, heart rate, absorption, and emptying of the bowel and bladder, autonomic neuropathy shows up with symptoms influencing the deficiency of control of these capacities. Symptoms might incorporate issues with the pulse, voiding, passage of stools (constipation or diarrhea), sweating, or heart rate.
Cranial neuropathy is like peripheral neuropathy, except that the cranial nerves are involved. Any of the cranial nerves can be included. One of the more common reasons for cranial neuropathy is the loss of bloodstream from the optic vein to the optic nerve, reasoning ischemic optic neuropathy. Amyloidosis is one of the basic causes of this uncommon disorder.
A specific nerve can be associated with neuropathy. At the point when a particular nerve is included, the indications are restricted to the dissemination of that nerve. The most included peripheral nerve is the middle nerve at the wrist in carpal passage condition. Any peripheral nerve can get captured and the signs and indications of neuropathy. The ulnar nerve is regularly entangled at the elbow. The peroneal nerve is uncovered at the external part of the knee. Whereas the pudendal nerve can cause pain in the perineum and is assuaged by sitting on a latrine seat or an inflatable donut. The capture of the horizontal femoral cutaneous nerve at the midsection of the waist, called meralgia paraesthetica, causes numbness at the external part of the thigh.
- Peripheral neuropathy is a condition wherein the nerves in the peripheral nervous system become harmed.
- Peripheral neuropathy symptoms rely on the reason. Generally, the problem influences the nerves that give sensation, which causes pain, burning, and tingling signs of the nerves affected.
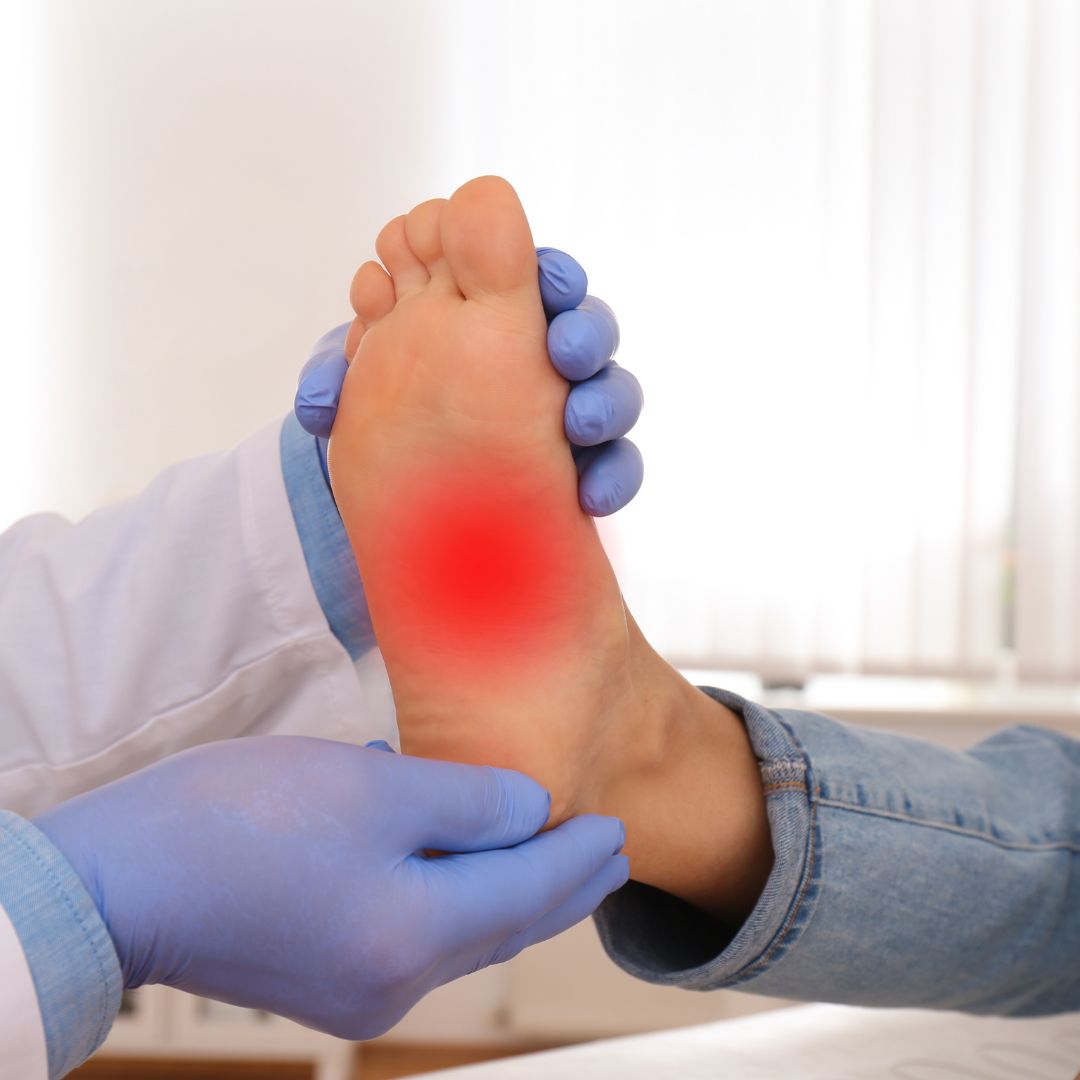
- Generally, peripheral neuropathy occurs in the hand and feet.
- Numerous different diseases and conditions can cause peripheral neuropathy, for instance, drugs, diabetes, vitamin deficiency, kidney failure, and shingles.
- Peripheral neuropathy is analyzed by tests, indicative and blood tests, and periodically skin biopsies.
- The treatment for peripheral neuropathy relies upon the reason; however, the prognosis for many other different diseases and medical problems that cause peripheral neuropathy can be effectively prevented and treated.
Symptoms
The symptoms of peripheral neuropathy fairly rely upon the reason. Generally, peripheral neuropathy influences the nerves of sensation. Subsequently, individuals with peripheral neuropathy foster pain, burning or tingling in the appropriation of the influenced nerves. Normally, this is in the feet and or hands. This can cause numbness, tingling, or burning in the fingers and toes.
At the point where shingles cause peripheral neuropathy, the nerve influenced causes severe burning and tingling sensation. For instance, the face, the buttock, at the side of the chest, and so forth.
Causes
There are numerous possible causes for peripheral neuropathy, including:
- Diabetes mellitus.
- Vitamin deficiency (especially B12 and folate).
- Shingles (postherpetic neuralgia).
- Liquor Consumption.
- AIDS, regardless of whether from the disease or its therapy, kidney failure, and syphilis.
- Autoimmune diseases that incorporate lupus, rheumatoid arthritis, or Guillain-Barre disorder.
- Inherited disorders, for example, Charcot-Marie-Tooth disease or amyloid polyneuropathy.
- Treating toxins like heavy metals, gold compounds, mercury, lead, arsenic, and organophosphate pesticides.
- Cancer treatment medications like vincristine (Oncovin and Vincasar) and different medications, for example, antibiotics that include metronidazole and isoniazid.
- Rare diseases like neurofibromatosis can prompt peripheral neuropathy. Other uncommon intrinsic neuropathies incorporate Fabry sickness, Tangier disease, hereditary sensory autonomic neuropathy, and hereditary amyloidosis.
- Statin prescriptions have been connected to peripheral neuropathy, even though neuropathy affected by statins only a rare causing symptom.
While postherpetic neuralgia and diabetes are the most common reasons for peripheral neuropathy, frequently no reason is found. In these circumstances, it is alluded to as idiopathic peripheral neuropathy.
Oftentimes, peripheral nerve entrapments, like carpal passage disorder, are viewed as peripheral neuropathies. In such cases, severe pressure on the nerve rather than a disease condition leads to nerve malfunction.
Treatment
The treatment for peripheral neuropathy relies upon its cause. The initial phase in treatment is to search for the actual reason.
- Vitamin insufficiencies can be revised.
- Diabetes can be controlled, even though control may not switch the neuropathy. The objective with diabetes is early identification and sufficient treatment to forestall the occurrence of neuropathy.
- Neuropathies that are related to insusceptible illnesses can improve with the treatment of immune system infection.
- Neuropathy affected by nerve ensnarement can be treated by active physical therapies, infusions, or medical procedures.
- Brief treatment with thoughtful infusions can limit the chance of shingles advancing to postherpetic neuralgia.
The pain of the neuropathy can typically be controlled with drugs. The most reliable treatment is over-the-counter drugs, like acetaminophen, ibuprofen, or anti-inflammatory medicine. Tricyclic antidepressants like amitriptyline (Elavil) or nortriptyline (Pamelor) and hostile to seizure drugs, for example, carbamazepine (Tegretol) have been utilized to soothe the pain of neuropathy. Capsaicin, the chemical for chili peppers is available over the counter as a cream to help reduce the pain of peripheral neuropathy. A prescription patch of 8% capsaicin (Qutenza) is approved for the treatment of postherpetic neuralgia. Pregabalin (Lyrica) is a medication that is used for the treatment of postherpetic neuralgia and diabetic peripheral neuropathy, while duloxetine (Cymbalta) has been approved for use in the treatment of diabetic peripheral neuropathy A prescribed solution of 7 percent capsaicin (Qutenza) is supported for the treatment of postherpetic neuralgia. In few cases, narcotics can be utilized to help control the pain that can be related to peripheral neuropathy.
Both alpha-lipoic acid and vitamin B6 are an option for relief in chemotherapy-induced peripheral neuropathy.
There is a progressive investigation into medicines for peripheral neuropathy, going from assessing the adequacy of topical gels to bone marrow medications. As this research advances, new therapies for patients can be expected.
People who believe that they have peripheral neuropathy must-visit for assessment since numerous reasons for peripheral neuropathy can be effectively treated.
Additional Information
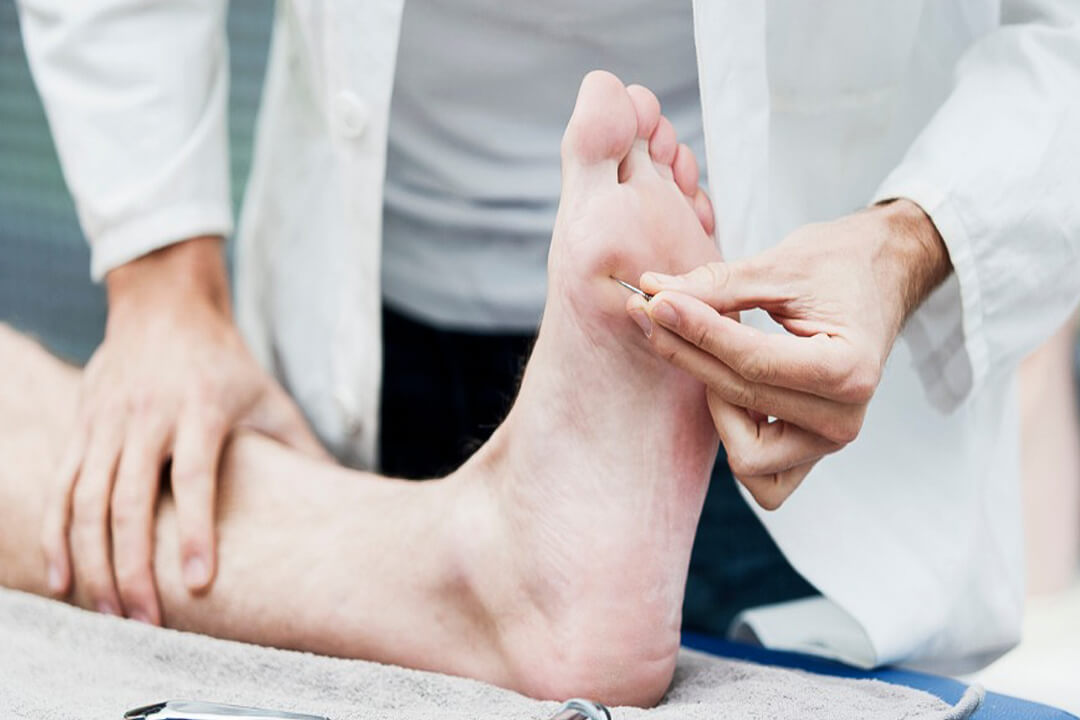
Since peripheral neuropathy has many causes and numerous presentations, the initial step to analysis is playing out an intensive medical history and physical assessment. Certain tests are performed during the physical assessment, including monofilament and vibration testing are precise in diagnosing specific types of peripheral neuropathy. Blood examination for exposure to toxins and electrodiagnostic study. For example, nerve conduction studies, and electromyography are also extremely valuable, albeit these examinations would not assist with the diagnosis of small fiber neuropathy. Skin biopsies or quantitative sudomotor axon reflex testing (QSART) is periodically used to help analyze small fiber neuropathy.